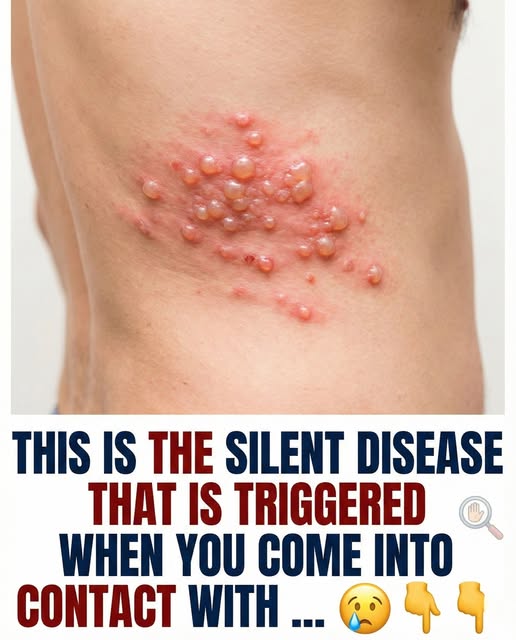
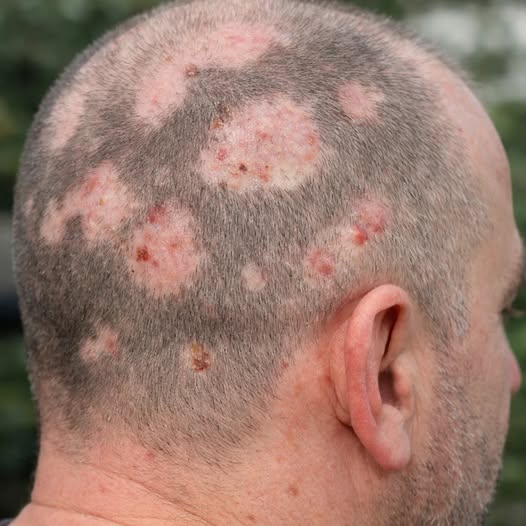
Shingles, medically known as herpes zoster, often causes alarm when it appears—largely because many people do not fully understand why it happens or what triggers it. Even individuals who consider themselves healthy can be surprised by how suddenly it begins. Although it is not always openly discussed, shingles is relatively common, especially later in life. Having a clear understanding of how shingles starts, which early signals to watch for, and how it typically unfolds can make a meaningful difference in recovery and long-term comfort.
Shingles is not a new or mysterious illness.
It is directly tied to the varicella-zoster virus, the same virus that causes chickenpox—an infection many people experience during childhood. After chickenpox clears, the virus does not leave the body. Instead, it remains quietly inside the nervous system, inactive for many years. In some individuals, it can stay dormant for decades without
Reactivation is more likely when the immune system becomes less effective.
Aging naturally affects immune function, which helps explain why shingles is more frequently diagnosed in adults over 50. Other contributing factors may include prolonged emotional stress, chronic health conditions, severe physical strain, or medical treatments that suppress immune activity. Major life events or periods of extreme fatigue may also create conditions that allow the virus to resurface. While older age remains one of the strongest risk factors, shingles can also occur in younger adults under the right conditions.
A key feature of shingles is that it often begins before a rash is visible.
Early symptoms can be subtle and are frequently mistaken for other issues. Many people experience localized sensations such as tingling, heightened sensitivity, burning, or a deep aching pain in one specific area. These feelings usually follow the pathway of a nerve and may appear several days before the skin shows any visible change. Because the area may look completely normal during this stage, the warning signs are easy to miss.
As shingles progresses, a rash typically emerges.
The rash most often appears on one side of the body or face and follows a recognizable pattern based on the affected nerve. Small, fluid-filled blisters commonly develop, along with redness and swelling. While the rash is often what prompts someone to seek care, medical professionals frequently note that pain can be the most difficult symptom. In some cases, the discomfort may feel sharp, stabbing, or intensely burning.
With timely medical attention, shingles often improves without serious complications.
Antiviral medications work best when started early—ideally within the first few days after symptoms begin. Early treatment can shorten the course of the illness, reduce symptom severity, and lower the chance of lingering nerve pain. When treatment is delayed, a complication called postherpetic neuralgia may occur. This condition involves ongoing nerve pain that can persist long after the blisters and rash have healed.
Postherpetic neuralgia can have a major impact on daily life.
People who develop it often describe persistent discomfort that disrupts sleep, affects concentration, and interferes with routine activities. The pain may last for months or longer, creating emotional strain in addition to physical distress. This is why healthcare providers emphasize recognizing early symptoms and seeking medical guidance promptly rather than waiting for the rash to fully appear or worsen.
Contagiousness is another common concern.
Shingles itself does not spread from person to person the way colds or flu do. However, the virus can be passed through direct contact with fluid from the blisters. If someone who has never had chickenpox or has not been vaccinated is exposed, they may develop chickenpox—not shingles. For that reason, extra caution is recommended around infants, pregnant individuals, and people with weakened immune systems during the active blister stage.
Prevention is now a major focus in shingles care.
Vaccines created to reduce the risk of shingles and its complications are widely recommended, especially for older adults and individuals with certain health conditions. These vaccines have been shown to lower the likelihood of developing shingles and to lessen symptom severity if it does occur.
Beyond medication, shingles also highlights the value of overall wellness.
Supporting immune health through balanced nutrition, adequate sleep, stress management, and attention to the body’s signals helps strengthen natural defenses. In many cases, the body provides subtle cues before a larger problem becomes obvious.
In summary, shingles is a well-established but often underestimated condition.
Understanding where it comes from, recognizing early warning signs, and responding quickly can greatly influence recovery and long-term comfort. Staying informed supports prevention, encourages timely care, and helps reduce the risk of prolonged pain or complications.